Artificial Insemination
It involves introducing sperm, previously treated in the laboratory, into the woman’s uterus or cervical canal, in the period close to ovulation, with the aim of achieving pregnancy.
What does Artificial Insemination involve?
Artificial insemination is an assisted reproduction technique that involves introducing sperm, previously treated in the laboratory, into the woman’s uterine cavity to achieve pregnancy. This way, it attempts to shorten the distance between the sperm and the egg, thus facilitating their encounter.
It is a simple and painless procedure, suitable for women with open fallopian tubes and correct ovarian function. The pregnancy rate per artificial insemination cycle is around 20-25%.
When is Artificial Insemination indicated?
AIC:
- Male indications:
- Decrease in the number or motility of sperm, and/or abnormalities of the same (mild or moderate oligozoospermia /asthenozoospermia /teratozoospermia)
- Difficulty of sperm penetration into the uterine cavity (abnormalities preventing intercourse and/or hindering ejaculation)
- Female indications:
- Anatomical or functional alterations of the uterus,
especially of the cervix (cervical or uterine factor). - Alterations in the menstrual cycle (ovulatory dysfunction).
- Endometriosis
- Anatomical or functional alterations of the uterus,
- Unexplained infertility:
- Couples where after the basic infertility study, the cause has not been found.
AID:
- Male indications:
- Absence of sperm in the semen
(azoospermia), provided it is not possible to recover sperm from the testicle and/or epididymis. - Severe decrease in the number or motility of sperm present in the semen (severe oligo and/or asthenozoospermia), sometimes after failure of in vitro fertilization.
- Certain chromosomal or genetic alterations without the possibility of preimplantation genetic diagnosis.
- Risk of transmission of other types of pathologies such as infectious diseases
- Absence of sperm in the semen
- Women without a male partner.
Requirements for Artificial Insemination

At least one open fallopian tube
Adequate motile sperm count (in case of AIC)

Not having previously undergone 6 or more insemination cycles
Artificial Insemination Process
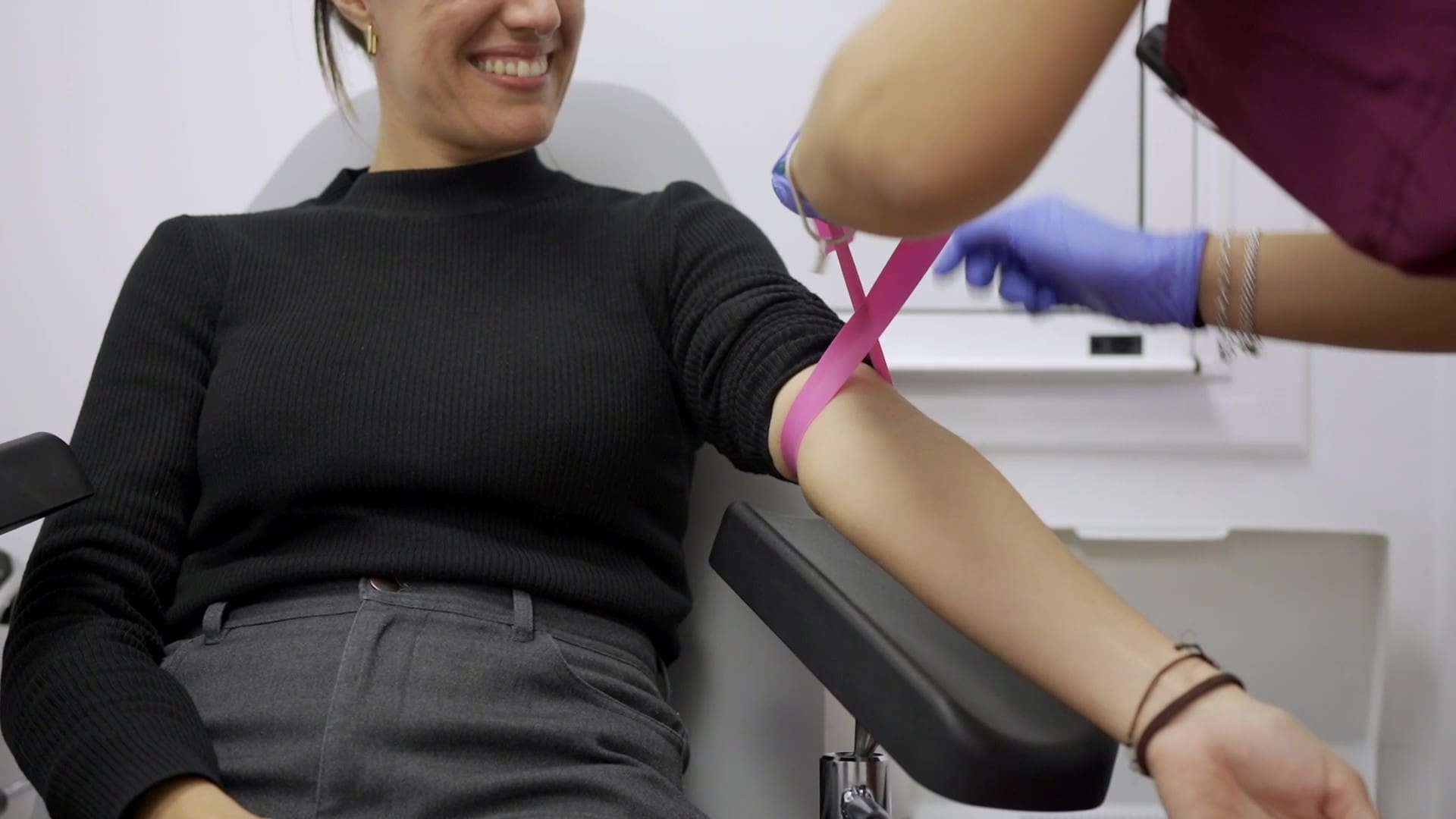
1. Request your first free visit
- Visit with an expert doctor in Assisted Reproduction.
- Fertility Study where we perform an ultrasound to evaluate the egg reserve and a semen analysis.
- Medical visit for results and diagnostic guidance.
2. Hormonal control and stimulation
Artificial insemination can be performed during a natural cycle, or after a process of ovarian stimulation. The pregnancy rate is significantly higher in stimulated cycles than in spontaneous ones.
Ovarian stimulation is performed using drugs whose action is similar to certain hormones produced by the woman called gonadotropins.
The purpose of this treatment is to obtain the development of one or several follicles, inside which an egg will mature.
Read more
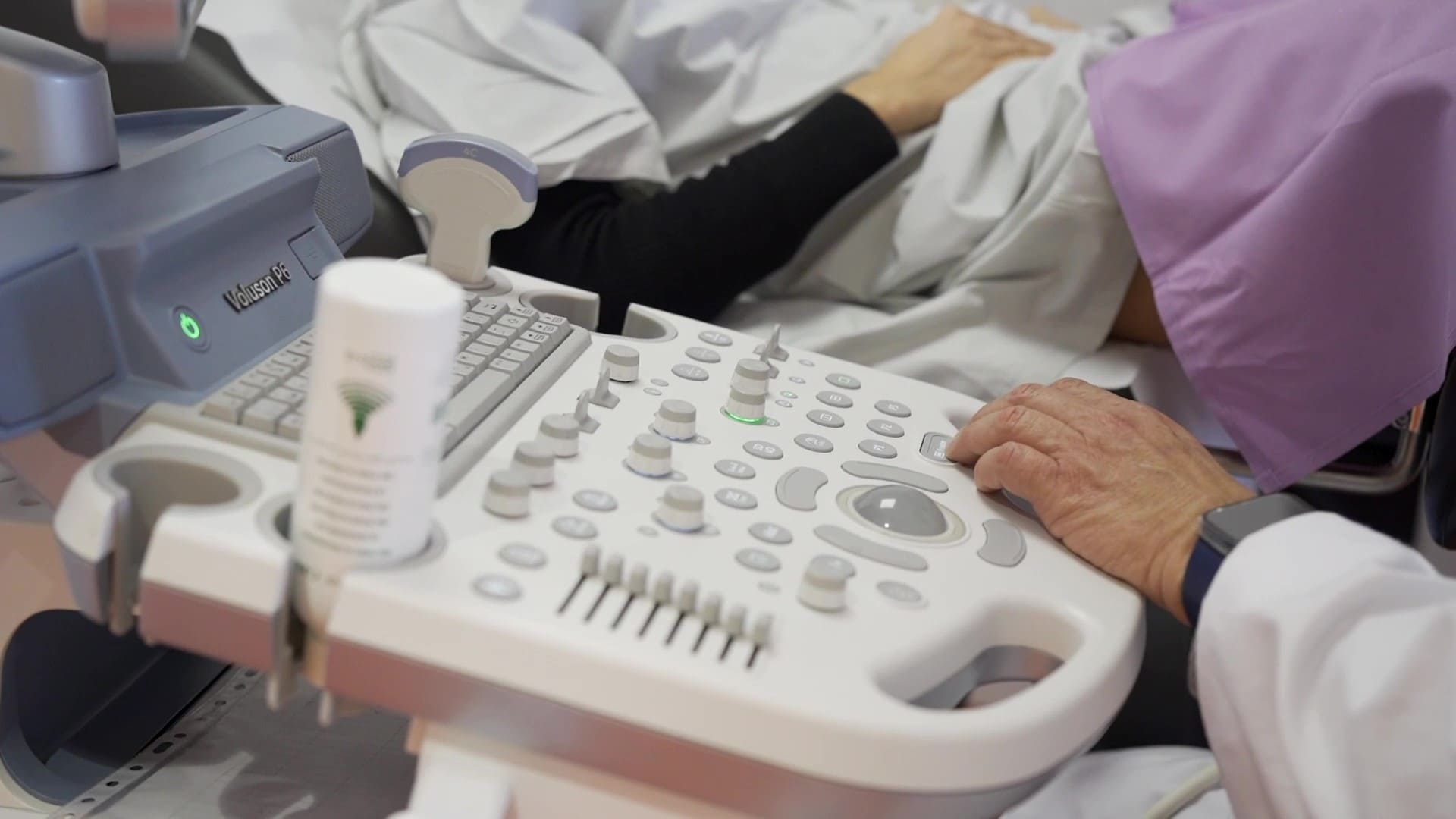
The stimulation process is monitored through serial vaginal ultrasounds that allow us to track the number and size of follicles, complemented with blood tests to know the levels of certain hormones (basically estradiol).
Stimulation usually lasts 10 to 14 days depending on the protocol used and each patient’s response to treatment. Once optimal follicular development is achieved, human chorionic gonadotropin hormone (hCG) is administered to induce oocyte maturation and follicular puncture is scheduled 34-38 hours later.
3. Medication
Currently, the most commonly used medications are injections, of subcutaneous application, which provide autonomy and comfort to patients.
The gonadotropin dose and the start day may vary depending on the case. The ovarian stimulation process is usually monitored through vaginal ultrasounds that inform about the number and size of developing follicles, as well as endometrial thickness, sometimes complemented with hormone determinations.
Read more
Once optimal follicular development is achieved, a medication (the hCG hormone) will be administered, whose action is similar to the luteinizing hormone (LH) that triggers ovulation, then scheduling the day and time of insemination.
It is very important to respect the indications provided by the center regarding the administration time.
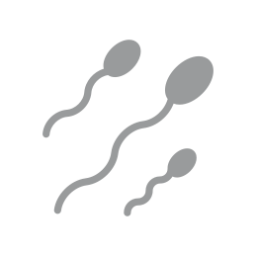
4. Andrology Laboratory
On the day scheduled for insemination, the andrology laboratory will proceed with the sperm capacitation of the partner’s semen sample (AIC) or the semen sample from the bank (AID) in order to select the best quality sperm.
The capacitation techniques aim to eliminate the seminal plasma from the ejaculate and select the sperm with better motility for insemination, eliminating immobile sperm.
5. The Insemination
Subsequently, in the gynecological consultation, these sperm are introduced into the woman’s uterus, using a thin and flexible catheter; this procedure is painless and does not require anesthesia or hospitalization.
The purpose of this procedure is to achieve the deposit of sperm as close as possible to the site of ovulation, thus avoiding the obstacles that the “hostile” environment of the vagina produces on sperm concentration and motility.
Read more
Finally, some hormonal treatment may be advised as support for the luteal phase, with the aim of favoring possible pregnancy.
After insemination, the woman can continue with her normal daily activity. Strict rest is not necessary after this procedure, although it is advisable to avoid physical exercises considered risky.
x days after insemination, a blood test will be performed to determine if a pregnancy is starting. Confirmation of this will be carried out with an ultrasound 15 days after the blood test.
Success rates for AIC and AID
Baby-at-home rate in artificial insemination cycles performed at Gravida between 2019 and 2022.
AIH (partner)
AID (donor)
Meet our specialists in Artificial Insemination

Dr. Anna Galindo Trias
Medical Director of Gravida

Dr. Carla Rojas Bautista
Specialist in Assisted Reproduction

Dr. Laura Gomila Villalonga
Specialist in Assisted Reproduction

Dr. Josep Maria Gris Martínez
Senior Associate Specialist at Gravida
Frequently Asked Questions
What is the difference between Conjugal Artificial Insemination (AIC) and Donor Artificial Insemination (AID)?
Conjugal Artificial Insemination (AIC) uses semen from the male partner, while Donor Artificial Insemination (AID) uses semen from a donor. AID is usually recommended in cases of severe male infertility or for women without a male partner.
How long does an Artificial Insemination cycle take?
The Artificial Insemination cycle usually lasts about 4 weeks. It includes ovarian stimulation (if necessary), ovulation monitoring, and insemination at the optimal time. Then, there is a waiting period of approximately 2 weeks to confirm pregnancy.
How many Artificial Insemination attempts are recommended before trying another treatment?
Between 3 and 6 attempts of Artificial Insemination are usually recommended before considering other fertility treatments, such as In Vitro Fertilization (IVF). However, the number of attempts may vary depending on the woman’s age and medical history. Consulting with a fertility specialist is key to making the best decision.
Is Artificial Insemination painful or does it have side effects?
Artificial Insemination is a minimally invasive procedure and generally painless. Some women may experience mild discomfort similar to menstrual cramps. Side effects of medication, if used, may include swelling or tenderness in the ovaries, but these are usually temporary.
Real opinions from our patients
Nos atendió la doctora Anna Galindo, una profesional increíblemente amable, cercana, siempre con una sonrisa, que te explica todo con claridad desde el primer momento. Nos pidió unas analíticas y, por suerte, todo salió bien.
En una visita rutinaria, me explicó con muchísima paciencia que estaba justo en mi periodo de ovulación y que, según los resultados, no necesitábamos ningún tratamiento complejo, solo un pequeño empujón con suplementos vitamínicos. Nos recetó unas vitaminas y, sinceramente, fue como magia… ¡ese mismo mes me quedé embarazada!
Recuerdo perfectamente que nos dijo con gran humildad: “Espero que no tengáis que volver aquí para ningún tratamiento.” Y así fue. Es una doctora que no busca venderte tratamientos innecesarios, como ocurre en otras clínicas, sino que apuesta por lo más natural y respetuoso con tu cuerpo.
También quiero dar las gracias a la doctora Laura Gomila, a quien conozco personalmente. Siempre ha estado pendiente, aconsejándome y resolviendo mis dudas con muchísimo cariño.
Recomiendo Grávida sin dudarlo, no solo por su profesionalidad, sino por el trato humano, la humildad y el amor con el que trabajan. Estoy profundamente agradecida por haber encontrado este equipo.
Partíamos de dos negativos de otra clínica, y encontrar esta clínica y esta doctora fue todo un acierto, nos hizo todas las pruebas necesarias para dar con el problema, lo tratamos, y bingo, nos quedamos a la primera! 😁 estamos muy muy agradecidas con el trato de todo el personal, pero en especial con el de nuestra doctora, que nos fue muy clara desde el minuto uno, y supo acompañarnos en este proceso que para nosotras no resultó fácil, por las experiencias anteriores! Ahora nos encontramos desbordantes de felicidad a la espera de la llegada de nuestro segundo bebé!
Por supuesto, hay pruebas que podríamos habernos hecho antes, pero este sigue siendo un área que aún no se ha explorado a fondo. Cada paciente tiene una situación muy diferente y cada médico tiene su propio enfoque. Mi esposa se embarazó después del segundo intento de FIV, y encontrar una solución fue un trabajo en equipo entre nosotros y Gravida.
Acudir a una clínica privada cuesta dinero, y la FIV es una experiencia psicológica difícil. Debe tener en cuenta que los ginecólogos responden a nuestras preguntas y nos orientan, pero la decisión de realizar más pruebas o tratamientos antes de la implantación depende de la paciente, por lo que debe participar.
Contacten con María, Noémi, Andrea… y con todos los que se me olvidan.
TODO EL EQUIPO, incluyendo a mi doctora Carla Rojas y a mi embrióloga Ana, todos extremadamente atentos y profesionales.
Mis ojos brillaron al instante.
Estaba súper feliz después de recibir la transferencia el lunes 13 de febrero de 2023.
Sentí todo después (mi implantación sobre las 18:20 y luego la implantación el jueves por la mañana) y mi cavidad seguía funcionando… 5 días después de la transferencia, quería saber si mis sensaciones eran reales. Por eso, el sábado 18 de febrero, me hice la prueba beta a las 10:00 y el resultado llegó por la tarde. Estaba temblando, tenía lágrimas en los ojos con 39 UI, lo que corresponde a mi implantación el jueves por la mañana (16 de febrero). 48 horas después, el lunes 20 de febrero (ayer), me hice otro análisis de sangre a las 10:00 y descubrí 161 UI. 😍 ¡Qué alegría! 🤩 ¡Por fin tengo a mi pequeño dentro de mí! Ha construido su nido, que terminará mañana, miércoles 24 de febrero, a la hora de la ovulación 14.
A todos, por cierto, hay un grupo en Facebook llamado “PmetteschezGravida”. No duden en unirse.
Gravida y su equipo estarán siempre en mi corazón.
Primera transferencia a los 46 años.
A todos: ¡CREA en ti mismo, pero sobre todo, hazlo con el equipo de Gravida! ❤️ ¡Son adorables! Sinceramente.
Nora, también conocida como Sibel Sara
Deseando que todo vaya bien para poder volver a verla y presentarle a nuestro bebé 🥰
La recomendamos 100%. Gracias por todo Laura 😘
En especial queremos agradecer a la Dra Galido por el trato directo con ella y a la Dra Rojas que nos atendió en ocasiones puntuales y nos hizo sentir igual de bien atendidas.
Ahora estamos en proceso de cumplir el sueño que tanto llevamos esperando. GRACIAS!
Después de más de 10 años luchando por ser madre, llegué por casualidad a la web de Gravida. No me arrepiento porque hoy soy mamá de un pequeño que tiene casi 6 meses.
Tuve un equipo muy profesional y atento. El protocolo salió bien a pesar de la distancia. Hubo muchos correos electrónicos y llamadas telefónicas pero valió la pena.
Mi pinchazo salió bien al igual que la transferencia. Estuviste atento a pesar de la barrera del idioma. Me sentí a gusto, no estresado ni ansioso.
Mi FIV funcionó en el primer intento en su hospital. Si bien tuve que enfrentar muchos fracasos inexplicables.
Hoy redescubrí la alegría de vivir mirando a mi hijo que me llena de felicidad.
Al tener embriones en stock estoy considerando un segundo embarazo.
Gracias a todo el equipo de Gravida. Gracias a ti gané mi lucha contra la vida por la vida.
Con toda mi sinceridad.
Ha sido un placer poder vivir ese proceso acompañada de ella, tanto por el trato como por la profesionalidad.
También estamos muy agradecidos con la atención recibida por parte de todo el equipo de enfermeras, embriólogas, y recepción.
¡Muchísimas gracias!
todo unas personas excelente. Yo estoy
mega feliz. No hay palabras para agradecerle este regalo a mi Dios, a Gravida y ami bb por escogerme. Full recomiendo la clínica Gravida
Muy agradecidos con todos!
Realizamos una fiv y durante todo el proceso se nos explico claramente en que consistía el proceso, y sobretodo fueron realistas con los porcentajes de éxito. Nos sentimos bien asesorados y acompañados.
Todo el personal es muy profesional, queremos agradecer especialmente a la doctora Gomila. Esperamos poder ir a presentarte a nuestro bebé.
Request your first free visit




